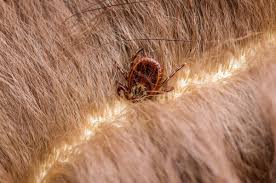
Here in Bellingham, many of us share the same routines — getting outside whenever we can, heading to the trails or the water, and bringing our dogs along for the ride (and sometimes our cats, too). As outdoor activity increases with spring and warmer weather, so does the chance of encountering ticks, including those that can carry Lyme disease, a bacterial infection caused by Borrelia burgdorferi.

Each May, Lyme Disease Awareness & Prevention Month offers a helpful reminder that tick exposure affects both people and pets, and that prevention and early recognition play an important role in protecting the whole family. Staying informed about Lyme disease and other tick-borne illnesses allows pet owners to take simple, proactive steps — and to recognize when something doesn’t seem quite right — so outdoor time can stay focused on enjoying the moment, not worrying about what might be missed.
Learn more about Lyme Disease Awareness & Prevention Month
Lyme Disease Basics: How Ticks Transmit Infection to Pets
Lyme disease is caused by bacteria that ticks transmit when they feed on a host’s blood. In the U.S., the black-legged tick is the primary vector for Lyme disease. Ticks must be attached and feeding for at least 24–36 hours before they transmit infection, so regular checks and removing ticks promptly are vital to reducing risk. Early prevention and identification of tick exposure is key to protecting pets.
Signs of Lyme Disease in Dogs
Dogs may become infected after a tick bite, but not all infected dogs show obvious symptoms. When clinical signs develop, they commonly
include:
- Limping or shifting lameness
- Swollen or painful joints
- Fever, lethargy, or decreased appetite
- Swollen lymph nodes
Left untreated, Lyme disease can in some cases lead to more serious issues such as kidney or heart involvement.
At BBVSH Bellingham, we pay careful attention to these clinical signs and diagnostic findings, because early recognition often allows for more effective treatment outcomes.
Lyme Disease in Cats: What We Currently Understand
Cats can be infected with the bacteria that cause Lyme disease, but this is much less common than in dogs, and evidence of clinical illness in cats is limited. Some cats may mount an immune response without showing signs; others may develop vague symptoms such as lameness, fever, or fatigue — but most do not exhibit noticeable illness.
Because cats groom themselves frequently and are generally less likely to carry heavy tick burdens, the overall risk of clinical Lyme disease in cats is considered low. However, this does not eliminate the need for vigilance during tick season, particularly for outdoor cats.
Preventing Lyme Disease in Pets: Medications and Everyday Strategies
Like many pet owners in our community, prevention often comes down to everyday habits — what we use, what we notice, and the small routines that help keep pets healthy while they enjoy the same outdoor spaces we do.
Prevention is the best strategy against Lyme disease. Here’s how veterinarians help protect pets:
Tick-Control Medications for Lyme Disease Prevention
Veterinarians recommend regular use of tick-control products, including monthly oral or topical medications that kill or repel ticks before transmission can occur. These products significantly reduce the chance that a tick will attach and begin feeding.
Vaccines for Lyme disease are also available for dogs (but not typically used in cats) and may be recommended based on geographic location and lifestyle. Your veterinarian can help determine whether vaccination is appropriate for your dog.
Daily Tick Checks and Outdoor Awareness
- Inspect your pet daily after outdoor time, especially in wooded or grassy areas
- Pay close attention to warm, protected areas such as ears, between toes, under the collar, and along the belly
- Limiting access to tall grass and brush can lower tick exposure
Tick Removal and Lyme Disease Risk: What to Do and When to Seek Help
Even with consistent prevention, ticks can occasionally attach to pets. Knowing how to remove a tick correctly — and when to seek veterinary help — can reduce the risk of Lyme disease and other tick-borne illnesses.
How to Remove a Tick From Your Dog at Home
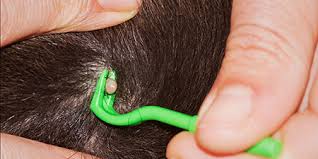
If you find a tick, remove it as soon as possible using fine-tipped tweezers or a tick-removal tool:
- Grasp the tick as close to the skin as possible, where the mouthparts enter the skin
- Pull straight upward with steady, even pressure
- Avoid twisting, squeezing, or crushing the tick
- After removal, clean the bite area and your hands thoroughly
Ticks generally need to remain attached for 24–36 hours before transmitting Lyme disease, so prompt removal significantly reduces the risk of infection.
If you are unsure how to remove a tick safely, cannot remove it completely, or notice redness, swelling, or discharge at the bite site, contact your veterinarian for assistance.

When Veterinary Help Is Recommended for Tick Removal
Veterinary removal is advised when:
- The tick is deeply embedded or difficult to grasp
- Mouthparts remain in the skin after attempted removal
- Your pet becomes lethargic, develops fever, or shows lameness following a tick bite
At BBVSH Bellingham, our team can safely remove ticks, evaluate the bite site, and advise on monitoring or testing based on your pet’s exposure and medical history.
Trusted Tick Removal Resources for Pet Owners
American Lyme Disease Foundation – All About Ticks
American Kennel Club (AKC) – Guide to Removing Ticks from Dogs
Diagnosing and Treating Lyme Disease in Pets
If Lyme disease is suspected, your veterinarian will use a combination of medical history (including known tick exposure), clinical signs, and screening tests to assess your pet.
Treatment typically involves a course of antibiotics. In dogs showing clinical signs, a four-week course of antibiotics such as doxycycline is often effective, with improvement in joint and limb symptoms often seen within days.
More involved treatment plans may be needed in complicated cases or when other organ systems are affected. Our internal medicine specialists are available for advanced diagnostics and tailored treatment protocols suited to each patient’s needs.
When Lyme Disease in Pets Requires Advanced Veterinary Care
Many pets exposed to ticks never develop illness, and when Lyme disease is identified early, initial treatment is often straightforward. However, some pets experience persistent symptoms or develop complications that require deeper evaluation.
Referral to a veterinary internal medicine specialist may be appropriate when:
- A pet tests positive for Lyme disease and continues to show clinical signs despite treatment
- Symptoms such as lameness, fever, or lethargy persist or recur
- There is concern for organ involvement, including the kidneys, nervous system, or heart
- Diagnostic findings suggest immune-mediated or systemic effects of infection
At BBVSH Bellingham, our board-certified internal medicine specialists focus on the diagnosis and treatment of complex disease. Using advanced diagnostics and a case-by-case approach, we evaluate how Lyme disease may be affecting the whole body and work closely with your primary care veterinarian to ensure coordinated, comprehensive care.

Female Rocky Mountain wood tick, Dermacentor andersoni
Photo: James Gathany, CDC
Living Well With Pets During Tick Season
Spending time outdoors with pets is part of what makes living in this area so special. Staying mindful of ticks, keeping up with prevention, and paying attention to subtle changes in how your pet feels or moves can go a long way toward catching problems early.
Lyme disease can be a serious concern, but with awareness, preventive care, and timely treatment, it is a manageable condition for most pets. And when symptoms linger, don’t quite fit the pattern, or begin to affect more than just the joints, having access to advanced evaluation can make a meaningful difference.
If your primary care veterinarian has recommended further assessment — or if you’re worried that something more may be going on — the team at BBVSH Bellingham is here to help. As part of this community, we’re committed to supporting pets and the people who love them, so they can continue to enjoy life outdoors, season after season.
Ticks and Other Diseases That Can Affect Pets
While Lyme disease is one of the most well-known tick-borne illnesses, ticks can transmit multiple other diseases that affect pets, several of which are relevant to the Pacific Northwest.
Depending on the tick species and geographic area, dogs — and more rarely cats — may also be exposed to:
- Anaplasmosis, which can cause fever, joint pain, lethargy, and low platelet counts
- Ehrlichiosis, associated with bleeding disorders, immune suppression, and chronic illness
- Rocky Mountain spotted fever, a potentially serious disease that can affect multiple organ systems
- Tick paralysis, a rare but serious condition caused by toxins in tick saliva
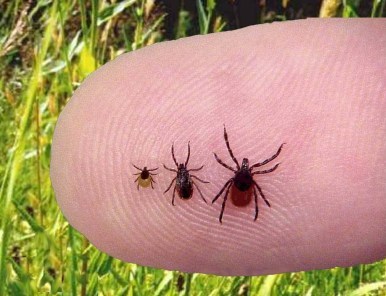
In the Pacific Northwest, pets are most commonly exposed to ticks such as the western black-legged tick (Ixodes pacificus) and the Rocky Mountain wood tick (Dermacentor andersoni).
Because many tick-borne diseases share similar symptoms — such as fever, lameness, lethargy, or appetite changes — diagnostic testing is often needed to determine the underlying cause when pets become ill after tick exposure.
For pet owners interested in learning more, these trusted resources provide detailed, veterinarian-reviewed information:
- American Veterinary Medical Association (AVMA) – Tick-borne disease and outdoor animal guidance
- Merck Veterinary Manual – Tick-borne diseases in animals
Frequently Asked Questions About Lyme Disease in Pets
What is Lyme disease in pets?
Lyme disease is a tick-borne bacterial infection caused by Borrelia burgdorferi. It can affect pets, especially dogs, after being bitten by an infected tick. The disease may cause joint pain, fever, and lethargy, and in some cases can lead to more serious complications if left untreated.
How do pets get Lyme disease?
Pets get Lyme disease from the bite of an infected tick, most commonly the black-legged tick. Ticks usually need to be attached and feeding for 24–36 hours before transmitting the bacteria, which is why regular tick checks and prompt removal are important.
What are the signs of Lyme disease in dogs?
Common signs of Lyme disease in dogs include limping or shifting lameness, swollen or painful joints, fever, lethargy, decreased appetite, and swollen lymph nodes. Some dogs may not show symptoms right away, while others develop signs weeks or months after exposure.
Can cats get Lyme disease?
Cats can be exposed to the bacteria that cause Lyme disease, but clinical illness in cats is uncommon. Most cats do not show obvious symptoms, though some may develop vague signs such as lethargy, fever, or lameness. Tick prevention is still important for cats, especially those that spend time outdoors.
Is Lyme disease common in the Pacific Northwest?
Ticks capable of transmitting Lyme disease and other tick-borne illnesses are present in the Pacific Northwest. Pets in this region are most commonly exposed to ticks such as the western black-legged tick (Ixodes pacificus) and the Rocky Mountain wood tick (Dermacentor andersoni), which can carry different pathogens.
How can I prevent Lyme disease in my pet?
Preventing Lyme disease includes using veterinarian-recommended tick-control medications, performing daily tick checks after outdoor activity, avoiding tall grass and brush when possible, and discussing Lyme disease vaccination for dogs with your veterinarian if appropriate.
What should I do if I find a tick on my dog?
If you find a tick on your dog, remove it as soon as possible using fine-tipped tweezers or a tick-removal tool. Grasp the tick close to the skin and pull straight upward with steady pressure. Clean the area afterward. If you’re unsure how to remove the tick safely or if your pet develops symptoms, contact your veterinarian.
When should I contact a veterinarian after a tick bite?
You should contact your veterinarian if you’re unable to remove a tick completely, if the bite site becomes irritated or infected, or if your pet develops symptoms such as fever, lethargy, or lameness after a tick bite.
How is Lyme disease diagnosed in pets?
Lyme disease is diagnosed using a combination of medical history, physical examination, and diagnostic testing. Veterinarians may use screening tests to detect exposure and recommend additional testing if clinical signs or complications are present.
How is Lyme disease treated in dogs?
Dogs with clinical signs of Lyme disease are typically treated with a course of antibiotics, often for about four weeks. Many dogs show improvement in joint pain and fever within days of starting treatment, though more complex cases may require additional evaluation.
When does Lyme disease require a veterinary specialist?
Referral to a veterinary internal medicine specialist may be recommended if a pet has persistent or recurring symptoms, tests positive and does not respond as expected to treatment, or shows signs of complications involving the kidneys, nervous system, or other organ systems.
Can ticks transmit other diseases to pets besides Lyme disease?
Yes. Ticks can transmit several other diseases that affect pets, including anaplasmosis, ehrlichiosis, Rocky Mountain spotted fever, and, in rare cases, tick paralysis. Many of these conditions share similar symptoms, which is why diagnostic testing is important when pets become ill after tick exposure.
Why is May important for Lyme disease awareness?
May is Lyme Disease Awareness & Prevention Month, a time to highlight the importance of tick prevention, early recognition of illness, and education for both people and pets as outdoor activity increases during warmer months.
References:
- Merck Animal Health: Tick-borne diseases
- Merck Manuals: Ehrlichiosis and anaplasmosis
- Merck Veterinary Manual: Tick paralysis in animals
- Merck Veterinary Manual: Tick removal
- American Lyme Disease Foundation
- American Lyme Disease Foundation: Tick identification and information
- AKC: How to remove a tick from your dog
- AKC: Ticks on dogs
- Dermacentor andersoni (reference)